


YES, past Medicare and Centrelink benefits do have an impact on medical negligence claims.
Compensation received in medical negligence claims may also affect the injured persons ongoing rights and entitlement to Centrelink.
IMPORTANT: -
Yes, if treatment and other Medicare benefits such as nursing and home care benefits have been obtained for injuries sustained as a result of medical negligence these expenses will form part of the medical negligence claim as a head of damage called “past medical expense”.
Yes, while expenses paid by Medicare are claimable as a head of damage in medical negligence, the compensation received at settlement for past medical expenses cannot be kept by the injured party as this would constitute a double up of compensation.
Therefore, the money claimed for past Medicare must go back to Medicare and/or the private health fund.
Upon request, Medicare will issue a Medicare History Statement from the date of injury to date of request. This statement will detail every expense paid by Medicare over that period.
The injured party will need to tick the box next to treatment that relates to any injuries sustained as a result of the medical negligence. This form is then returned to Medicare.
Following which, Medicare will issue a Medicare Notice of Charge which provides a total figure to be paid back to Medicare when the matter settles.
If a Medicare Notice of Charge is not available or has expired at the time of settlement then 10% of the settlement money will be deducted by the Insurer and sent to Medicare.
Medicare will then send a Medicare History Statement to the injured party, upon receipt of the Medicare History Statement, Medicare will determine the charge and withdraw the charge amount and return the balance of the 10% to the injured party.
If there is no Medicare Charge the full 10% will be returned to the injured party.
Yes, if as a result of medical negligence the injured party is unable to work and has obtained a Centrelink benefit the injured party may need to reimburse Centrelink at the end of the medical negligence claim.
If an injured party is unable to work, their past economic loss will form part of the medical negligence claim as a head of damage called “past economic loss”.
If the injured party is compensated for their past loss of income they will not be able to keep that compensation and the Centrelink benefit for the same period as this would constitute a double up of compensation.
If a portion of the settlement money relates to past economic loss, Centrelink will be notified and will issue a clearance or charge.
The clearance will advise of any amounts owing to Centrelink for any benefits that are compensation affected.
It is important to note, if the injured party has unpaid Centrelink debts (e.g. garnishee or unpaid child support) those debts may be payable from the medical negligence compensation.
If there is an amount to be reimbursed to Centrelink, the Insurer will deduct the amount owed to Centrelink form your settlement money.
An insurer is unable to pay out any settlement money until a Centrelink clearance or charge is received. Generally this process takes between four 4-12 weeks.
If no Centrelink benefits have been claimed over the relevant period Centrelink will issue a Clearance stating there is no charge and no money will be deducted by the Insurer for reimbursement.
YES, in some circumstances.
If a portion of the settlement money represents loss of income an injured worker may be precluded from obtaining Centrelink benefits into the future.
A preclusion period applies irrespective of whether the injured party has previously received Centrelink.
It is important to note, preclusion period may affect entitlements to Pensions and other age benefits.
The injured party will be advised of any Medicare and/or Centrelink reimbursements as well as any Centrelink preclusion periods prior to the resolution of their medical negligence claim.
However, it is important to be open and frank about past Medicare and Centrelink benefits and debts to ensure the claim runs smoothly and the right amount of compensation is obtained at the resolution of the medical negligence claim.
To read more about medical negligence damages see our recent blog post: “4 MOST COMMON DAMAGED CLAIMED IN MEDICAL NEGLIGENCE MATTERS”.
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
Medical Law © 2020 Privacy & Disclaimer

Anyone who has been subject to medical care and/or treatment that falls below the expected standard of care and as a consequence has sustained injury may be entitled to make a medical negligence claim for compensation.
In Australia, the different states and territories have different threshold in relation to the extent of injury and damages. These thresholds may restrict an injured persons entitlements to make a medical negligence claim.
Medical negligence claims can be made against a number of medical institutions and providers including but not limited to: -
Medical negligence claims can be brought in relation to a number of failures, including but not limited to: -
Medical negligence claims are notoriously complex and are strongly defended by the medical negligence insurers.
In order to be successful in medical negligence the injured party must prove with evidence that the health care provider has breaches their duty of care (negligence) and that breach caused injury (causation).
This evidence must satisfy certain legislative requirement. If the elements of negligence and causation are not made out in the evidence, the claim will not succeed.
Due to the complex nature of medical negligence claims, and the importance of expert evidence it is always best to have an expert medical negligence lawyer act for the injured party so that the best result can be achieved in a timely manner.
Yes, most medical negligence lawyers will enter into a no win no fee costs agreement at the commencement of your claim.
This means that the law firm will fund the claim up until the resolution of the matter. This is beneficial to injured parties as often they are struggling financially and would not otherwise be able to fund the claim.
No win no fee means that if the injured party is not successful in their claim, legal fees will not be charged.
When the claim is successfully resolved the lawyer will charge for the work undertaken and the expenses paid during the claims process.
That being said, in medical negligence claims, if successful, the medical negligence insurer will often pay approximately 70% of the legal fees, with the remainder payable by the injured party.
The process for an injured party is summarised as follows: -
Generally, 98% of medical negligence claims settle outside of Court in the alternate dispute resolution process E.g. Compulsory Conference and/or Mediation.
If a claim does not settle at Compulsory Conference/Mediation and is required to be litigated it does not mean the claim will proceed all the way to “Court” and a hearing.
Usually, matters that are required to be filed in Court do not make it to a hearing. This is because, in the lead up to a hearing there are plenty of opportunity to resolve the claim by way of negotiation.
In QLD, the pre-court procedure requires parties to take a number of steps prior to meeting at a Compulsory Conference to try and resolve the claim.
Generally, a matter should proceed to a compulsory conference and resolution 12-18 months after the negligent party is put on notice of the claim.
To read more about medical negligence damages see our recent article here.
In QLD, there are strict time limits in which to make a medical negligence claim.
Under the Limitation of Actions Act 1974 an injured person has three (3) years from the date the cause of action arose in which to bring a claim.
Extensions are available in some circumstances but are difficult to obtain.
Therefore, it is important that medical negligence claims are commenced in Court prior to the expiry of the limitation period.
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
Medical Law © 2020 Privacy & Disclaimer
OVERVIEW
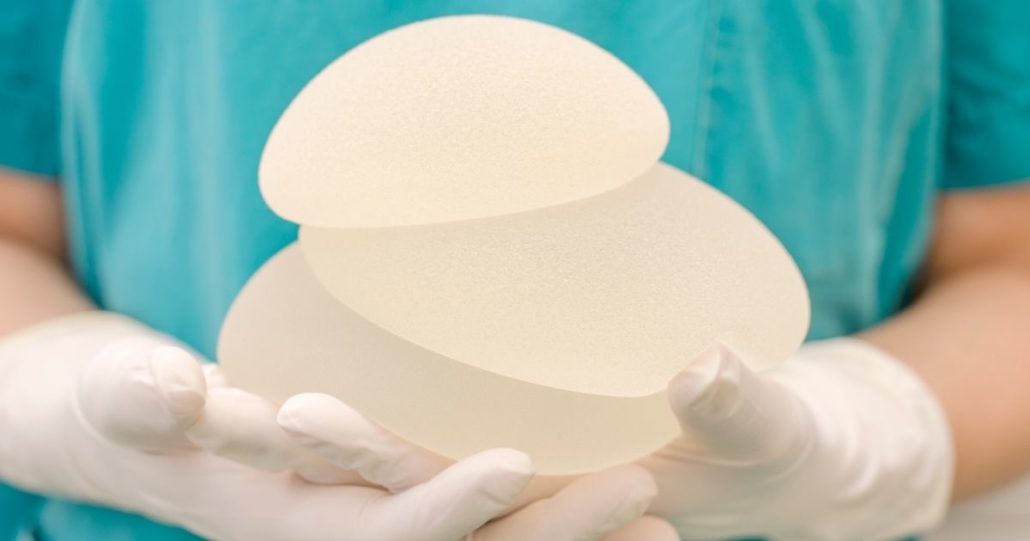
A link has been identified between the use of breast implants and expanders and BIA-ALCL.
Research has identified that patients with textured implants are at greater risk of developing BIA-ALCL than those with smooth implants. However, data suggest some BIA-ALCL cases have been caused by smooth implants.
Unfortunately, in Australia, it has been established that most implants utilised in breast surgery procedures have been textured implants.
Due to the increase in patients developing BIA-ALCL, health warnings have been issued to patients who have breast implants and may be at risk of developing BIA-ALCL.
In early 2021, the Therapeutic Goods Administration (TGA) was made aware of at least 76 cases of BIA-ALCL, this number is expected to grow as more women come forward with symptoms.
It appears a number of women who have been diagnosed with BIA-ALCL have had their implants for a number of years, with symptoms only developing more recently.
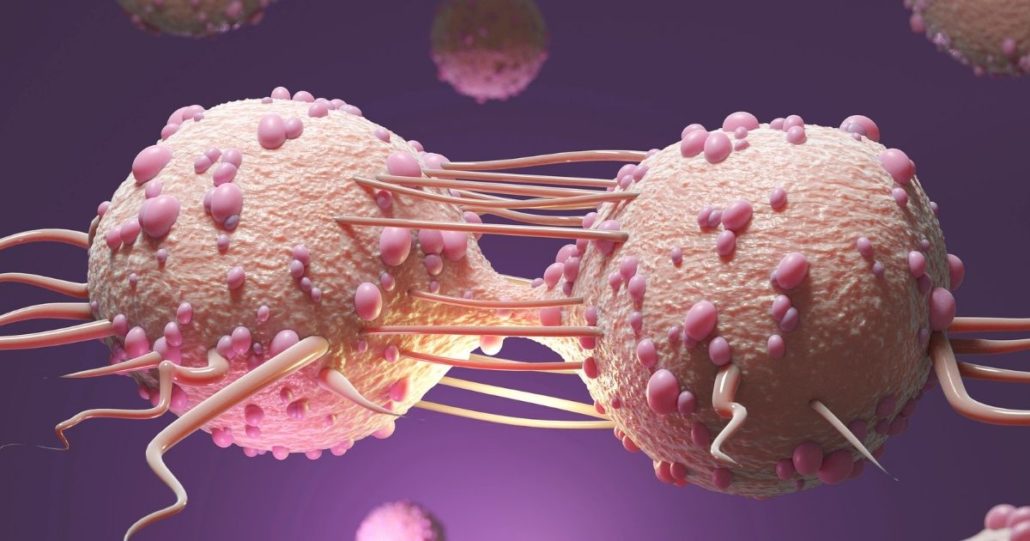
Breast Implant Associated Anaplastic Large Cell Lymphoma is a form of non-Hodgkin’s lymphoma.
The BIA-ALCL is found in the scar tissue and fluid surrounding the implant product. The cancer is usually contained in this pocket, however, if left untreated the cancer can spread to other parts of the body.
BIA-ALCL symptoms include but are not limited to: -
If patients with breast implants experience any of the above symptoms, they should report their symptoms immediately to a health care professional so investigation can be undertaken as soon as possible.
If patients have concerns and/or symptoms they should immediately contact their health care provider to discuss their concerns and/or symptoms.
If diagnosed early, most cases of BIA-ALCL can be treated with surgery to remove the implant and scar tissue. If detected and treated early, treatments such as radiotherapy and chemotherapy may be avoided.
For this reason, it is vital that if patients have concerns or are experiencing symptoms they consult a health care professional for immediate investigation.
While it is said the majority of implants utilised in Australia in recent years have been textured, some patients may not be aware of their type of implant used in their procedure.
If patients wish to confirm the type of implant utilised they should contact the specialist/hospital they attended for the implant procedure.
The specialist/hospital will have retained the product stickers for the implant in their records which will specify the product manufacturer and whether the implant is smooth or textured.
WHAT TO DO NEXT
If a patient believed that they have textured implants or BIA-ALCL they should:-
To read more about TGA recalls see our recent article: “TGA Recall Notices: What you need to do if you have received one”
For further information consult the TGA website: https://www.tga.gov.au/
Disclaimer: This article does not constitute medical or treatment advice. Always speak to a registered health care professional for medical and treatment advice.
References:
Medical Law © 2020 Privacy & Disclaimer
IF YOU HAVE RECEIVED A TGA RECALL NOTICE, YOU SHOULD:
The Therapeutic Goods Administration, otherwise known as the TGA, is the medical regulatory body in Australia that regulates the supply and use of therapeutic goods and medical products in Australia.
These goods and devices include: -
From time to time the TGA is notified of a therapeutic good or product that does not meet the required standard in Australia. When this occurs, the therapeutic good or product is recalled.
The recall is aimed to keep the community safe by withdrawing the good or product from the market and notifying those that may have already been affected by its use.
A recall occurs when a problem is identified with a product already on the market and in use.
Some of the reasons why a product is recalled included, but is not limited to circumstances where the product is: -
For a therapeutic good or product to be recalled by the TGA significant investigation and testing must have been undertaken prior to its withdrawal from the market. Therefore, all therapeutic goods and product recalls should be taken seriously and acted upon by affected patients immediately.
You may receive a recall notice, or you may be notified by your GP or specialist that a therapeutic good prescribed or a product utilised in your care is subject to a recall.
If you receive a recall notice or are advised of a recall you should: -
McInnes Wilson Lawyers has been made aware of TGA investigations into the link between textured breast implants and breast implant associated anaplastic large cell lymphoma (BIA-ALCL) and will provide further information on the developments of the investigation and impact on patients in our next article.
If you believe you have textured implants, you should urgently consult your treating GP or specialist for advice.
For further information consult the TGA website: https://www.tga.gov.au/
Medical Law © 2020 Privacy & Disclaimer
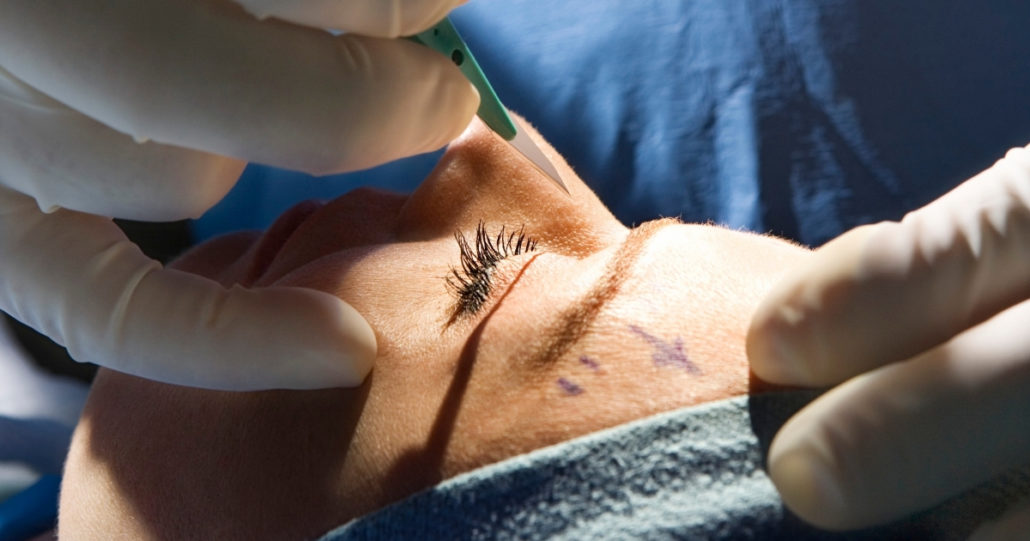
Briefly put, YES.
In Australia, there is a significant difference between the practice of plastics and cosmetic surgery, and between plastic surgeons and cosmetic surgeons.
All Australians seeking cosmetic surgery should be informed of the difference between specialist plastic surgeons and cosmetic surgeons and the differing standards and level of treatment of the two prior to undergoing any cosmetic procedures.
KEY TAKEAWAYS
The difference between plastic and cosmetic surgeons in Australia comes down to three core elements: -
In Australia, Plastic surgery is recognised as a field of speciality by the medical boards in Australia.
This means, to have a title of “plastic surgeon”, the surgeon would have undertaken 12 years of medical training, including five (5) years of surgical training, and be admitted to the medical board of Australia as a Fellow in plastic surgery.
Once accredited as a “plastic surgeon” the surgeon must undertake mandatory ongoing training and development throughout their career to ensure best practice.
Plastic surgeons are specialists who often undertake plastic and cosmetic surgery in hospital or private clinical settings, all of which are regulated and subject to strict health and safety, and sterilisation and Infection control protocols.
“Cosmetic Surgery” is not a field of speciality in Australia.
Generally, cosmetic procedures can be undertaken by medical practitioners such as Doctors and Registered Nurses.
While there is a two year cosmetic surgery program which can be undertaken by medical practitioners, this program is NOT accredited by the Medical boards in Australia.
Undertaking this program does not make a practitioner a specialist. This program is also NOT mandatory to perform cosmetic procedures.
This means cosmetic surgery and cosmetic procedures can be undertaken by doctors with a medical degree and nurses with a three year nursing degree.
There is significant difference between the skills, experience and expertise of a plastic surgeon and a practitioner undertaking cosmetic procedures.
Further, cosmetic procedures are often undertaken in private practice such as cosmetic clinics and clinics in shopping malls.
These clinics are not subject to the same health and safety and infection protocols and standards as hospitals or private specialist clinics.
There are a number of risks of cosmetic procedures when undertaken in private practice by practitioners: -
as cosmetic procedures in private practice in Australia are not regulated.
Noting that there are reasons for regulating treatment that involves your largest body organ.
Therefore, it is important for anyone contemplating undergoing a cosmetic procedure to be fully informed of the procedure, and of the skills, training and qualification of the practitioner undertaking the procedure.
THings to consider before undergoing a cosmetic procedure:
NOTE: Many “cosmetic surgeons” misrepresent themselves as specialists as they have undergone the additional two year training course, which is simply incorrect and may constitute fraudulent behaviour.
If following a cosmetic procedure a patient is unhappy with the outcome and has suffered ongoing injury, loss, and damage, they may be able to bring a medical negligence claim against the practitioner and obtain compensation for their injuries.
To learn more about damages in medical negligence claims, see our book on calculating damages here:
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
Medical Law © 2020 Privacy & Disclaimer

The Office of the Health Ombudsman (‘OHO’) is Queensland’s health service complaints agency. This system was set up to handle complaints in Queensland about health service providers. If you or a family member are unhappy with treatment or medical advice you have received by a health care provider, you are entitled to make a complaint.
Their main objectives are to:
Overall, the OHO’s role is to protect all Queenslanders in the provision of health services.
You can make a formal complaint about any health service, health service provider or practitioner, anywhere in Queensland. This includes registered and unregistered health practitioners.
This not only includes doctors, but also nurses, optometrists, dentists, chiropractors, occupational therapists, osteopaths, physiotherapists, nutritionists, massage therapists, naturopaths, homoeopaths, dieticians, speech pathologists and social workers.
You can also make a complaint against a public or private health care facility, such as a hospital, private clinic, ambulance service, mental health service and community health services.
You can complain about any aspect of healthcare services that you received. This includes the following:
Yes.
Before making a formal complaint, it is recommended that you talk to your health care provider.
Being up front about your concerns and asking questions is often the most effective way to solve your complaint. This can also lead to a resolution much quicker. You can do this in person or you could write a letter to your health service provider.
However, sometimes medical treatment may not be acceptable. In these cases, if you are not happy with the response you receive from your treating practitioner or this conversation is too upsetting, you can proceed with making a formal complaint to the Health Ombudsman.
You can complete an online health service complaint form and submit this online. Alternatively, you can print the complaint form and return as follows:
Alternatively, you can phone 133 646 and complain over the telephone or attend the Brisbane office.
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
Medical Law © 2020 Privacy & Disclaimer

When consulting with a doctor you have a right to feel: -
As patients, we have the utmost trust and faith in our doctors and treatment providers. An integral part of the doctor patient relationship is open communication and honesty. We tell our doctors things we would never tell anyone else, and we place our trust in our doctors to provide advice and undertake appropriate investigation and management.
Given the nature of this relationship, it is clear the doctor patient relationship is one which is inherently unequal.
Doctors have an ethical and legal obligation to make sure their patients feel safe, informed, and comfortable when receiving care and treatment.
Unfortunately, some doctors and medical providers use their position of power to exploit their vulnerable patients for their own gain.
Given the vulnerability of patients in this relationship, it is important that patients be aware of what constitute a breach of the doctor’s guidelines and the doctor patient boundaries.
Generally speaking, behaviours that would constitute a breach include, but are not limited to: -
Both the AMA and AHPRA have identified the issues surrounding patient consent to enter into sexual/intimate relationships with their treatment providers.
The issue with consent stems from the influence a doctor has over a patient and whether that consent is in fact informed consent, whether the patient has capacity, and whether the treatment being provided by the doctor could be expected to influence the patient’s decision making.
Relationships with former patients are also considered to be a breach of the guidelines as it is considered that the influence and power imbalance of the doctor patient relationship could extent long after the doctor ceases treating the patient.
Most patients who have been exploited by their doctors do not know what has occurred until sometime later as patients rarely understand what constitutes a breach of the guidelines and legal obligations of doctors and treatment providers.
In other circumstances there is a delayed recognition of breach by patients due to patient: -
The delay in recognition is very common due to the nature and circumstances of the relationship.
Unfortunately, a breach of the boundaries can have detrimental effects on patients including: -
If these circumstances sound familiar, and it appears there has been a breach of the doctor patient relationship the patient may be entitled to bring a medical negligence claim against that doctor.
By bringing a medical negligence claim against the doctor the patient may be entitled to compensation for the injury, loss, and damage sustained as a result of that breach.
To find out more on medical negligence damages, see our blog post: 4 MOST COMMON DAMAGES CLAIMED IN MEDICAL NEGLIGENCE MATTERS & WHAT THEY MEAN FOR YOU.
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
Medical Law © 2020 Privacy & Disclaimer

Inherent in all patient and medical provider relationships is a duty of care to provide reasonable care and skill when treating a patient. This duty extends to any actions taken, proposed to be taken or any decisions not to act at all.
This relationship exists between a broad range of medical providers and their patients including but not limited to; doctors, nurses, hospitals, and allied health professionals.
Generally, it is easy to establish that a duty of care relationship exists between medical providers and their patients.
Once the duty of care relationship is established, the next step is to prove the medical provider breached that duty and the standard of care.
After proving there has been a breach of the standard of care the next step is to prove that the breach caused harm / injury.
Otherwise known as causation, it will need to be established that the breached caused injury and harm that could have been avoided.
Relating the injury and harm back to the breach can often be challenging as there are usually other factors at play which have, at least in part, contributed to the injuries sustained.
This means that any ordinary rehabilitation or healing associated with the procedure / treatment undertaken must be distinguished from any additional injury and harm caused by the breach.
Once the harm / injury resulting from the breach is identified, the loss sustained must be identified in order to claim compensation.
When it comes to putting a value on the loss caused by the breach, the following should be considered: -
Calculating damage as a result of breach can often be challenging as there are a number of “heads of damage” to consider which include general damages, economic loss, medical treatment, and domestic assistance.
While compensation for injury and loss will not put the injured party back in the position they were in prior to the breach occurring, the compensation received will certainly assist with injury maintenance and healing, and help the injured party find closure and focus on the future.
Therefore, it is very important to properly assess the damages in medical negligence claims so an appropriate amount of compensation can be obtained for the injury sustained.
To find more information on the damages you may be entitled to see out blog article: 4 MOST COMMON DAMAGES CLAIMED IN MEDICAL NEGLIGENCE MATTERS & WHAT THEY MEAN FOR YOU.
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
Medical Law © 2020 Privacy & Disclaimer

In medical negligence in order to be successful in your claim, you must prove with evidence that the defendant owed you a duty of care, breached that duty of care, and as a result of that breach caused you injury, loss, and/or damage.
If you are successful in establishing a breach you will be entitled to compensation for your injury, loss, and/or damage.
The compensation you receive is assessed under heads of damages.
The four (4) most common heads of damages are: -
General Damages: In QLD, general damages are calculate on an “injury scale value” (ISV) as per the Civil Liability Act 2003 QLD.
The ISV scale ranges from 1 – 100 with 100 representing the most severe damage.
The ISV that you are assessed at is entirely dependent on the injuries you have sustained.
General damages are payable on a scale up to the maximum of $398,700 which is reserved for the most serious of injuries.
Your ISV must be assessed by an expert which your lawyer will arrange for you.
Non-Economic Loss (NSW): In effect, non-economic loss represent a pain and suffering as a percentage of a most extreme case (MEC).
Non-economic loss is only payable for injuries of at least 15% of a most extreme case as per the Civil Liability Act 2002 (NSW).
Ultimately, the compensation you are entitled to receive depends on the individual needs and circumstances of your case and will take into consideration elements such as; your suffering, the extent of your injuries, disabilities, and damage, your future prospects, and generally the impact your injuries have on your quality of life.
If as a result of your injuries you have had to take time off work, reduce your work capacity or ceased work in its entirety, you can claim compensation for your loss.
Your economic loss claim can be made in relation to your past and expected future economic loss including the associated loss of superannuation.
All claims for past economic loss must be supported with evidence such as, payslips, tax returns and medical certificates.
Claims for future economic loss must be supported by expert evidence setting out the nature and extent of your injuries and disabilities and the impact they have on your future employment. Your lawyer will arrange for you to be assessed for economic loss.
These damages include any treatment or expenses you have incurred in the past as a result of your medical negligence injuries. Past treatment and out of pocket are expenses are only claimable with evidence. Therefore, it is important you keep all receipts so you may recover your expenses.
Tip!
Damages are also payable for your future medical treatment for the remainder of your life. Your claim for future treatment will be based on expert opinion. Your lawyer will arrange for you to be assessed for your future medical treatment needs.
If as a consequence of your injuries you require care and assistance undertaking your usual daily duties, domestic tasks, or self-care and personal hygiene needs you may be entitled to claim damages for care and assistance.
Care and assistance is compensable on both a gratuitous (provided by friends and family) and commercial (paid) basis.
In order to claim damages on a gratuitous basis, a friend of family member must be providing care and assistance for a minimum of six (6) hours per week for a minimum of six (6) months.
All claims for gratuitous care and assistance must be supported by evidence. The type of evidence required to support your gratuitous care and assistance claim could be; a calendar showing rotations/shifts of family and friends providing assistance, a schedule of care and assistance, or a statement by the person providing that gratuitous care and assistance.
Claims for paid care and assistance in the past must be supported with evidence such as receipts for payments for services. If you are paying for care and assistance, make sure you keep your receipts in a safe place so you can provide them to your lawyer to support your claim.
All future paid care and assistance will need to be supported with expert evidence detailing your injuries, associated symptoms, and restrictions, and how they affect your day to day life.
Usually your lawyer will arrange for an assessment by an Occupational Therapist (OT) to discuss your ongoing care and assistance needs.
KEY TAKEAWAYS
To learn more about damages in medical negligence claims, see our book on calculating damages here:
One download between you and your key to compensation...
Want to fast track the process with our free interactive workbook?
If you are not sure whether to bring a medical negligence claim and wish to know what damages you would may be entitled to you should contact Medical Law for a free case assessment.
Medical Law © 2020 Privacy & Disclaimer

THREE THINGS TO REMEMBER WHEN VISITING YOUR GP
In Australia, general practitioners are the primary port of call for our general health maintenance and are more often than not, the first person we consult for our health concerns.
Many of us attend the same general practitioner for years, we often refer our loved ones and form a close relationship with our GP’s. Due to the nature of the doctor patient relationship we tend to form a high level of trust in the treatment and advice they provide as medical professionals.
In any relationship between a doctor and patient a duty of care exists. As a general practitioner, a duty of care is owed to the patient to: -
While this is not an exhaustive list, it is clear that a general practitioner must act in accordance with the duty of care at all times during their professional practice. This duty cannot be waived on the basis of a longstanding doctor patient relationship. The duty must be upheld in all circumstances.
It was established in Rogers v Whitaker (1992) 175 CLR 479 that practitioners must warn their patients of any risks that would be of significance to that particular patient. Prior to undertaking any procedure, your GP must first warn you of the associated risks and provide your informed consent.
It is important to know that even if a consent form is signed by a patient, very little weight is given to that consent form if a patient can prove they were not appropriately advised of the particular risk of that procedure, or if their GP failed to advise of alternative treatments that may be better suited to that particular patient and their circumstances.
That being said, if consent is given for a procedure that falls outside a general practitioners scope of practice and qualification, it is irrelevant if consent is given as that treatment would be considered a breach of duty of care.
It is of the upmost importance for general practitioner to recognise the limit of their experience and qualification while practicing in their professional capacity as general practitioner in Australia, as well as the significance of informed consent.
McInnes Wilson Lawyers have been investigating claims in which patients have trusted and accepted the advice and treatment recommendations of their GP and have consented to treatment which their practitioners did not hold qualifications in Australia to undertake, and which fell outside the scope of practice in Australia resulting in the patients suffering loss, damage, and disability.
Our investigations concern patients who attended upon their general practitioner for excision of sun damaged skin/lesions and/or moles. Generally excision for biopsy is a small surgical procedure which is not considered high risk and can be undertaken by an appropriately trained general practitioner.
In this case, following the return of the initial biopsy results the general practitioner proceeded to recommend and undertake a large excision and graft to the patient’s chest. Subsequently the tissue became necrotic resulting in permanent scarring and disfigurement.
Our experts have advised that the general practitioner breached their duty of care by offering a surgery that was firstly incorrect, and secondly an extensive procedure that fell well outside the scope of general practice.
This type of extensive surgical procedures should be undertaken by appropriately trained specialists in plastic surgery or specialist dermatologist as recognised by AHPRA.
Further, our experts advised that to perform such an invasive and extensive surgery in a general practice environment was not only inappropriate but also increased the risk of complications such as infection.
These cases raise important issues about the scope of a general practitioners practice and what treatment falls within the scope of a GP practicing in Australia.
Generally speaking, a general practitioner’s practice in clinics is limited to: -
What is certain is that extensive surgical procedures do not fall within the scope of general practitioners practicing in Australia, and should not be undertaken in general practice clinics.
If your GP is offering services over and above what would be considered a minor procedure, or if you are recommended treatment on a highly visible area such as your hands, décolletage, neck, or face, you should seek a second opinion from an appropriately trained medical specialist.
If you feel the advice you received from your general practitioner falls outside the qualifications and scope of practice of a general practitioner you should seek a second opinion.
KEY TAKEAWAYS
Medical Law © 2020 Privacy & Disclaimer